
Singapore Expo’s Covid-19 care facility. Source: Surbana Jurong.
To meet rising demands for medical care while relieving the pressure on public hospitals during the COVID-19 pandemic in mid-2020, the Singapore government converted several large- scale non-medical venues into Community Care Facilities (CCFs) to house COVID-19 patients who did not require acute medical care. Collectively, venues such as the Singapore Expo, Big Box shopping malls in Jurong and the Changi Exhibition Centre were able to house 17,000 stable patients. While the medical staff to patient ratio was reduced in these facilities, pharmacy support was imperative in enabling smooth supply and use of medications, as with any medical setting! Currently, some of these CCFs have dovetailed to other similar facilities to cope with the community surges and some facilities have also been converted to Community Treatment Facilities. However, workflows remain largely similar.
In this issue of Pharmacists in the COVID-19 Pandemic, we are honoured to interview five pharmacy staff, as they share their experiences in the running of pharmacies in the CCFs, and how it was like counselling the COVID-19 patients there (more affectionately known as “residents”). The pharmacy colleagues interviewed are:
- Chee Hov (Pharmacy Technician) and Isabelle (Senior Pharmacist) from Woodlands Health Campus (WHC)
- Chwee Huat (Principal Pharmacist) from Alexandra Hospital (AH)
- Rachelle and Stephanie (Pharmacists) from Singapore General Hospital (SGH)
What were your initial reactions towards having to help set up the CCF?
Chee Hov (WHC): Mixed feelings of nervousness and excitement. It was an honour to be part of the pioneer team running the CCF. It was both a meaningful and fulfilling experience to be part of the team fighting the pandemic!
Isabelle (WHC): Stressed! As I was unsure of the things that needed to be done and whether we could complete those tasks on time.
Chwee Huat (AH): Was very glad to have been offered the opportunity to contribute to the nation’s fight against COVID-19! And I was not alone – in fact, many of my colleagues were also very supportive, helpful and passionate about supporting the setup of the CCF. As the amount of work requires additional support beyond the pharmacy team, I was worried initially. But this was soon allayed by the many volunteers who stepped forward: from non-public health institution-based pharmacists to other folks with no pharmacy experience.
Rachelle and Stephanie (SGH): The team was initially anxious as there were a lot of uncertainties regarding the pandemic situation. The timeline was also very short to set up a facility of such scale and re-deploy existing staff from the hospital to run pharmacy operations at CCF. However, we were also excited as this was something completely new to many of us. It was also an opportunity to contribute by answering the nation’s call to fight against the pandemic.

Pharmacists from AH (Ming Liang, Chwee Huat and Ilya) who were involved in setting up of the Big Box CCF – described by Chwee Huat as his “fellow comrades” in the national fight against COVID-19
What were the key operational roles that pharmacy played in running of the CCF?
Rachelle and Stephanie (SGH): The key responsibility of the pharmacy at CCF was to ensure safe and timely supply of medications to its residents. The team was tasked to:
- Review and set up the drug list in GP Connect (GPC) at CCF to facilitate the prescribing of medications.
- Manage drug inventory in the pharmacy and clinics.
- Establish work processes to receive drugs from the hospital and supply drugs into the quarantine area, to minimise unnecessary staff exposure to the virus.
- Counsel residents on the use of their medications and any potential side effects through video counselling.
- Provide drug information services to doctors and nurses.
Chwee Huat (AH): GPC was the main electronic medical record system used in the management and care of the residents at the CCF. Hence it was important that the GPC was set up as a simple and easy solution for doctors and nurses to learn and use in a short span of time. This is especially important as the doctors and nurses who had volunteered were from very different backgrounds, with varying understanding of medication ordering systems. As the medical post sees scores of residents in a short span of time, the focus was on efficiency.
Pharmacists played key roles in coming up with the proposed formulary of the CCF, and liaised with doctors on the standard order instructions and bundled packs available for efficient prescribing, to cut down the number of data entries and promote user-friendliness. Once these were harmonised, pharmacy teams quickly got into action to start the pre-packaging and pre-labelling of drugs in standard pack sizes or bundles.
The result was that doctors, nurses, pharmacists and pharmacy technicians were able to dispense and counsel the CCF residents on the use of the medications efficiently as everything had been prepared.
Isabelle (WHC): Pharmacy was in charge of all things related to medications. Because of this, we were involved in a myriad of tasks: from the procurement of medications directly from vendors, coming up with workflows for on-site and off-site medication ordering and supply, to working with Integrated Health Information Systems to ensure that the clinic system was able to support our needs (for doctors to order safely and for us to use as a pharmacy and inventory management system), to the translation of medication-related information.
Chee Hov (WHC): My main responsibility was to ensure sufficient medication stocks both in the pharmacy store and across the CCF halls. I also ensured that the storage temperature was optimal. In addition, I was also involved in medication dispensing for residents who were uncontactable through the phone.
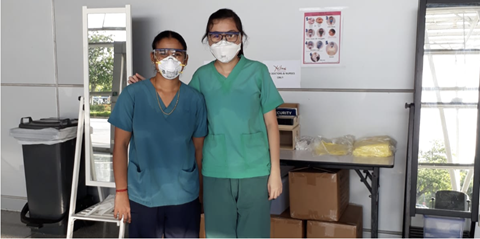
WHC pharmacist Isabelle with her non-pharmacy colleague at the CCF – evidence of bonds forged among newfound friends as they worked together for a common purpose of supporting the nation’s fight against COVID-19
Were there any challenges faced when communicating with other healthcare providers?
Chwee Huat (AH): I think there weren’t any challenges in communication with the other healthcare providers. On the contrary, the teamwork was great! The entire journey from the setup to the running of the CCF had blurred the lines between the stakeholders, where we thought more of how to make things work for each other and achieve the best possible care for our residents at the CCF.
Isabelle (WHC): As all of us were mostly working with each other for the first time, it took a while for us to adapt to each other’s working style. But once we warmed up to each other, it was easy to work as a team as we all had a common goal, which was to ensure that the patients receive the best care we can provide, using the resources that were available.
Rachelle and Stephanie (SGH): There were not many challenges faced when communicating with other healthcare providers at CCF as everyone was there for a common goal, i.e. to provide the best care for the residents at the facility. Some of the challenges encountered were during the initial period where everyone was getting used to the new work processes. However, this was quickly resolved with frequent huddles and discussions with the relevant parties.
Chee Hov (WHC): Not really. We were able to communicate effectively!
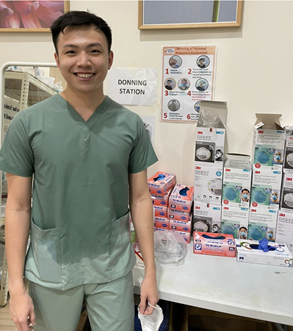
WHC Pharmacy Technician Chee Hov all smiles and ready to start the day by putting on his N95 at the donning station
How is the patient population different from your practice setting and were there any challenges faced when caring for this group of patients?
Isabelle (WHC): While the bulk of them had no past medical history, there was a group of residents who had undiagnosed hypertension or uncontrolled diabetes. Hence the doctors had to start them on oral anti-hypertensives or adjust their diabetic mediations while they stayed at the CCF. There was another group of residents with existing chronic conditions who used to get their medications from their home countries, but because of COVID-19, they were unable to obtain top-ups due to flight disruptions. The challenge was to ensure the continuation of care for these patients after they were discharged from CCF.
Chee Hov (WHC): Residents in CCF were mostly construction workers from overseas. I don’t think language was a barrier here, because they were able to understand simple English and we could supplement with gestures which we usually do in hospitals too. When needed, there were also colleagues to help with translation. Regular reassurance was given to let the residents know that they are going to be okay as they were very concerned with being hosts of COVID-19 virus. They miss their home too.

Migrant worker getting tested for COVID-19. Source: Reuters.
Chwee Huat (AH): Unlike in the hospital setting, the majority of the folks were not able to speak or read English fluently. To help them understand what the medications are for and how to take them, the pharmacy teams prepared multilingual labels for all medications. The labels consist of pictograms in languages spoken/read by the residents, ranging from Bengali, Hindi, Chinese, Thai, to Vietnamese and so on.
Rachelle and Stephanie (SGH): The patient population at CCF was completely different from the usual patients we encounter in the hospital. They were mainly young and healthy migrant workers, where most of them do not have any co- morbidities. As such, the clinical aspect of caring for them was generally more straightforward.

Use of Temi robots to reduce exposure of healthcare staff to patients. Source: Singapore General Hospital
Nevertheless, there were still challenges in providing care to them. This included the language barrier, cultural differences as well as emotional support needed. It was even more challenging to overcome all these when we were dispensing to them in full personal protective equipment (PPE) with limited facial expression. Fortunately, we managed to implement video counselling through Zoom and Temi robots, which enabled us to communicate with the patients without full PPE, from outside the quarantine area. We were able to communicate more effectively, with hand gestures and the use of pictograms to show the indications of the medications. In addition, video counselling enabled us to teach the residents administration techniques of devices such as inhalers and nasal drops, which would have been difficult to do so inside the quarantine area. We have also noticed that these patients required more reassurance and emotional support during medication counselling as they may be restless and anxious due to the quarantine period and pandemic situation in their home countries, as well as the different health practices.

The enthusiasm and cheer of pharmacy staff could not be hidden behind the layers of personal protective equipment that had to be donned for hours.
Could you share with us a memorable encounter from your experience working in the CCF?
Chee Hov (WHC): The most memorable part was that all of us from different backgrounds (different ages, different institutions etc.) were able to come together with one common mission and vision: to overcome this pandemic. Everyone was helping and supporting each other!
Rachelle and Stephanie (SGH): The most memorable experience which we’ve encountered at the CCF would be the camaraderie amongst the other healthcare professionals and support staff. As we typically work alone in the pharmacy, the others would frequently offer to get food for us or check in to make sure we were doing fine.
Although it was a period of uncertainties, it was heartening to see everyone from various backgrounds coming together to run the facility, working together to provide care to the residents. The residents were also appreciative of our efforts, despite our interactions being limited to broken English and hand gestures.
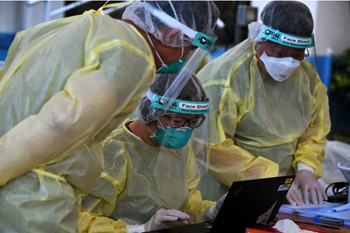
Healthcare workers working together. Source: Straits Times.
Isabelle (WHC): Expo CCF was the first big project that WHC worked together as a team on the same site, as we are all currently nested in different hospitals.
Chwee Huat (AH): The entire journey of setting up the CCF pharmacy and establishing the work processes with volunteers, doctors and nurses was very memorable indeed. I was very fortunate to have the help from many people: AH pharmacy folks who stepped up voluntarily to help in the training and setting up of the CCF pharmacy as well as repackaging of medications; fellow friends from WHC (Pei Chean and Isabelle) and SGH (Soo Boon and Jielin) who were so willing to share their experience in setting up the CCF pharmacy as well as the multilingual pictogram labels; volunteers who staffed the CCF pharmacy and bore the brunt of it all, and last but not least the fellow AH comrades who sacrificed their blood, sweat and tears to setup the CCF in a very short time span.
It was really heartening to see so many people from different clusters, backgrounds and teams working together in the fight against COVID-19.
A heartfelt “Thank You” to all of them!
Contributed by PSS Hospital Chapter.
*Disclaimer: All photos were taken in compliance with COVID-19 safe distancing measures at that point in time.


